|
Extracorporeal Shockwave Therapy (ESWT) has evolved from a puzzling treatment modality to a clinically proven technique utilised by physiotherapists since its inception in the 1980s. Initially deployed to obliterate kidney stones, this technology pivoted in the 1990s, focusing its high-energy acoustic pulses on addressing musculoskeletal disorders and tendinopathies. As research unfolded, its applications in treating various musculoskeletal dilemmas expanded, and institutions like Acland Street Physiotherapy have become adept at discerning suitable candidates for Shockwave Therapy.
Understanding the Healing Mechanism of Shockwave Therapy Despite being potentially undervalued due to its somewhat enigmatic nature, Shockwave Therapy operates on a thoroughly researched mechanism. The therapy deploys high-energy acoustic pulses or shockwaves, emanating from an ESWT unit, to stimulate small fibres. This activation, in turn, fortifies the body’s serotoninergic system, reducing nerve pain signals dispatched to the brain, and propels healing through enhancing local blood flow and metabolic reactions by breaking down calcifications and ameliorating the body’s inherent healing and pain management systems. Conditions Addressed by Shockwave Therapy Shockwave therapy proves its mettle by not only enhancing pain management and mobility but also by improving bone density and breaking down scar tissue, offering a non-surgical and non-invasive remedy for numerous conditions.
Navigating Through a Shockwave Therapy Session Prioritising the accurate identification of suitable patients and conditions for ESWT is pivotal, and Acland Street Physiotherapy invests in a comprehensive assessment of candidacy following a precise diagnosis. Contrary to its somewhat intimidating name, Shockwave Therapy is generally painless, a testament to the evolution of the technology since its early, more discomforting days. The modern iterations used by clinics like Acland Street Physiotherapy no longer necessitate local aneasthetic. A typical session, lasting a mere 5-10 minutes, involves the physiotherapist employing the shockwave therapy handpiece onto the impacted area, meticulously transmitting shockwaves to facilitate healing. Patient feedback plays a crucial role in optimising the applicator position and treatment intensity. While Extracorporeal Shockwave Therapy provides an invaluable toolkit in managing several conditions, it isn’t a universal remedy. Its pros, cons, and future research areas, encompassing issues like temporomandibular joint pain and varying tendinopathies, continue to unfold. However, unraveling the mysteries of Shockwave Therapy begins with a simple conversation with your physio, exploring its applicability and potential efficacy for your condition.
0 Comments
Over the past 15 years practicing as a local physiotherapist, I have discovered through clinical experience 5 critical key factors which determine the success or failure of your physiotherapy treatment program. I would like to share them to all my prospective and existing patients as being aware of these can help increase the likelihood of the success of your physiotherapy treatment program at Acland Street Physiotherapy, at the very least!
The 5 critical key factors which determine the success or failure of your physiotherapy treatment program are: 1. Ensure you do as much research as you can about the physiotherapist you are considering to book in with. Unlike a GP, you will likely spend a lot more time with your physiotherapist so it is important that you will likely get along. Questions to consider include:
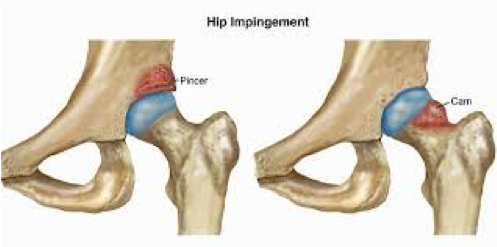
3. Work in collaboration with your physiotherapist to discuss your health goals, treatment options and timeframes. The physiotherapist should explain what treatment options will likely resolve the condition for you, and it is completely up to you on whether you feel comfortable about pursuing one or more options. There needs to be a clear plan in place to make treatment work for you. 4. Be prepared to do work. There is only so much benefit "hands on" passive treatment the physiotherapist can provide you as part of your recovery journey. It is arguably more critical that you actually complete the home exercise program the physiotherapist recommends for you to do. The physiotherapist should be designing a program that is realistic to you, and very well integrated into your lifestyle. 5. You should feel comfortable and not hesitate to communicate with the physiotherapist about your treatment program and any concerns outside the walls of the consult room. At Acland Street Physiotherapy, we encourage our patients to email the physiotherapist in between consultations, and on occasion, the conversation may be escalated to a phone call or an appointment if deemed necessary. Femoral acetabular impingement or "hip impingement" is a condition which involves abnormal contact of the hip joint between the ball of the hip and socket of the pelvis. The cause is generally multi-factorial which include childhood hip issues and repetitive strain or hip rotation. Clinical signs and imaging can confirm this diagnosis accurately. Patients often report pain and stiffness in the hip or groin area. Symptoms are often aggravated by squatting, climbing upstairs and prolonged sitting. This condition can respond well to physiotherapy treatment which may include manual treatment, strengthening and neuromuscular exercises. Surgery is often indicated as well as post surgical physiotherapy rehabilitation.
Early rehabilitation after an acute muscle injury can get you back to your favourite activities faster!
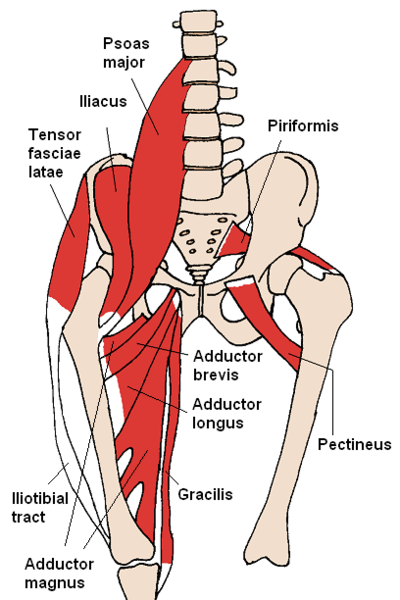
When you strain a lower limb muscle like a calf or a thigh, it is often possible to exercise or load these muscles up in the first couple of days right after the injury. Surprisingly, muscles can handle significantly more than you think in the first few days of a muscle strain. This recent study published in the New England Journal of Medicine supports this view. In conclusion, early physiotherapy rehabilitation after an acute muscle injury (even if it is severe), can help accelerate the healing process - allowing you to get back to your favourite activities much early than delaying professional intervention. Groin strains or tendinopathies generally occur with sports such as martial arts, football or ice hockey. The muscle belly-tendon part of the adductor tendon or where this tendon inserts to the pubic (hip) bone is generally tender when pressure is placed on it. The adductor longus muscle is the most commonly injured. Common risk factors to increasing the risk of injury the groin muscles include a weakness in adductor muscles and a core muscle weakness (tranversus abdominals).
The key differences between groin strains and tendinopathies are notably:
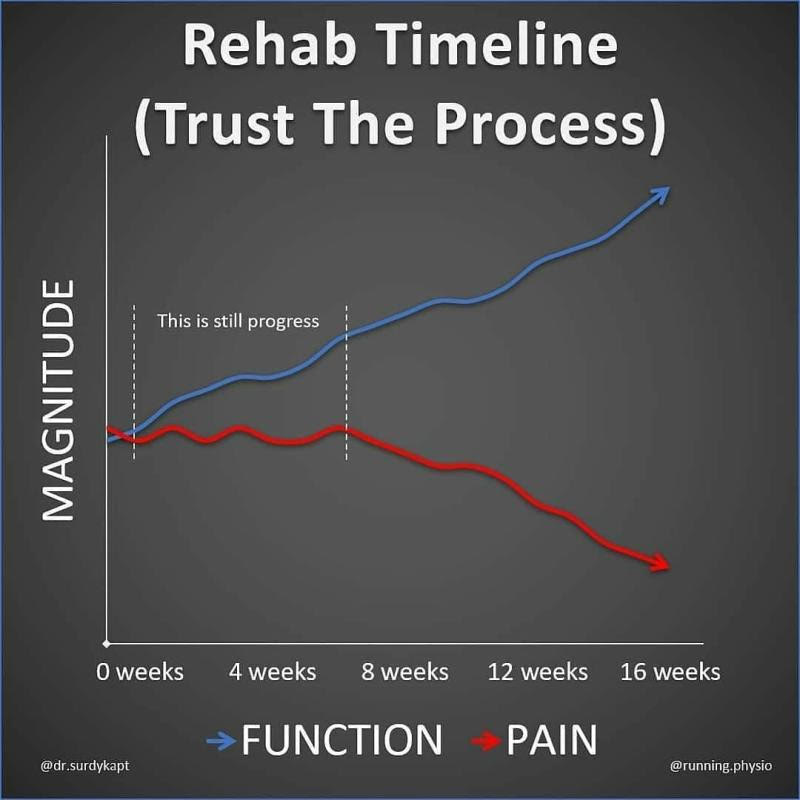
These injuries can respond very well to physiotherapy management which may include dry needling, manual therapy, extracorporeal shockwave, core stability, stretching and eccentric strengthening rehabilitation programs. Note for that groin related tendon injuries, exercise rehabilitation can take 3-6 weeks before full recovery can occur. Patience and persistence are the keys to a successful physiotherapy rehabilitation program for your injury or following orthopaedic surgery. At Acland Street Physiotherapy, we try our best to set very realistic expectations of full recovery from the beginning of the physiotherapy treatment program. We have a relatively low patient drop out out rate to injury rehab programs that need to be committed to for at least 3 months. We enlighten and train our patients from the beginning of the physiotherapy treatment program that their movement or function will improve much before pain does. Realistically, pain will most probably come on for the journey but will reduce over time. Nonetheless, in some cases, pain may resolve with a rapid increase in function.
It is important to understand that for some people depending on the nature of the injury, the pain will resolve completely. For most people, pain will continue on at a relatively manageable level. They will experience a little bit of a niggle or discomfort now and then and this might be the "new normal" moving forward. The key point here is that be reassured with a comprehensive injury rehabilitation program, you will with time, be able to return to doing the things you love, and your pain will be relatively less in all cases. In addition, completely resting and avoiding activities is often not the answer and can lead to poorer results in the longer term. During the COVID-19 pandemic, running observably has become an extremely popular exercise activity locally obviously, for its health benefits and simplicity as no equipment is required. I am avid runner myself recreationally often clocking up 50kms per week. Over the past 10 years as a physiotherapist, I have coached hundreds of my patients who have never ran before to shed a few pounds or improve their overall fitness. Many of my patients have misconceptions about running in particular, that running is bad for your knees and that you are at major risk of arthritis. This common concern has been debunked by science by multiple studies. Based on large population studies, the chances of developing arthritis from regular running are very slim. In fact, regular running has shown to strengthen joints and plays a protective role in the development of osteoarthritis later in life. Commonly reported knee pain by runners at Acland Street Physiotherapy that is generally treatable with a moderate amount of physiotherapy and strength training are Iliotibial Band Syndrome or Patellofemoral Pain Syndrome.
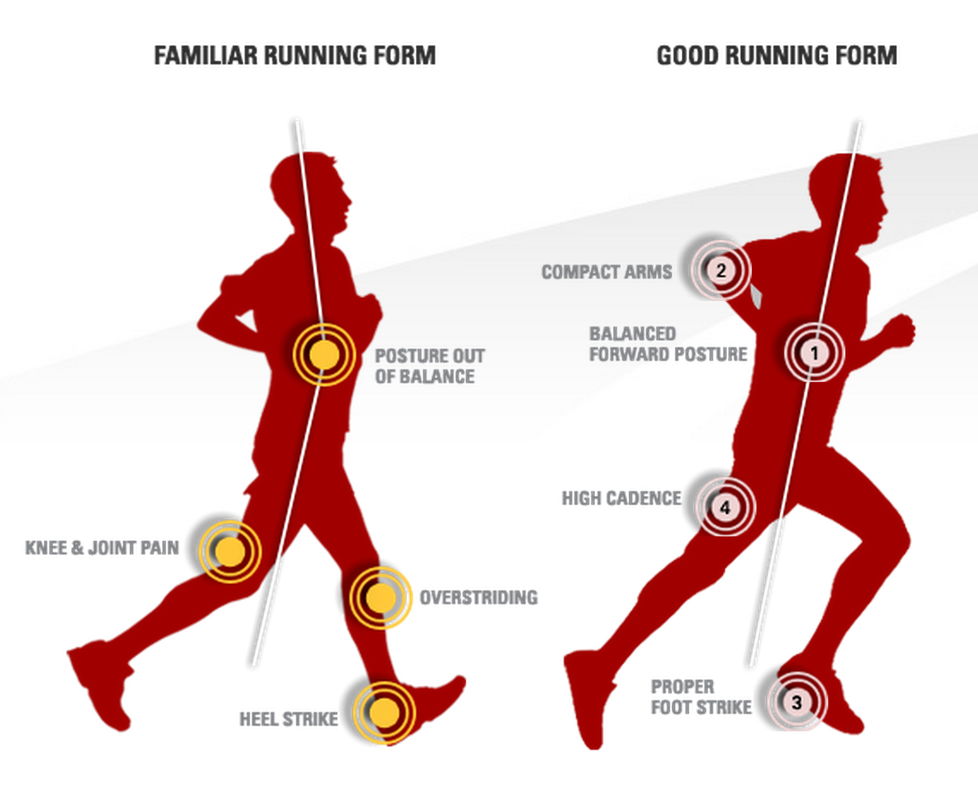
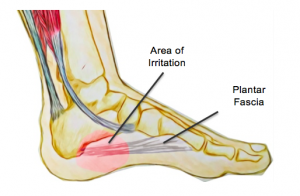
The following is a concise infographic on how what good running form generally looks like. If you would prefer to further explore this, please do not hesitate to make a booking with us for a comprehensive physiotherapy and biomechanical running assessment. Plantar fasciitis or "inner heel pain" can be a very painful condition that is the result of degeneration of the plantar fascia origin on the inside of the heel bone as well as the surrounding soft tissue supporting structures. The plantar fascia has a key role in providing arch support and shock absorption during weight bearing activities such as standing, walking and running.
It is often caused by an overuse or repetitive strain injury. Specifically, overuse causes micro-tears of the plantar fascia. Common risk factors include:
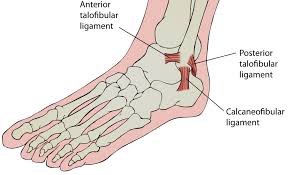
Before consider a cortisone injection, plantar fasciitis generally responds well to physiotherapy treatment including manual therapy, extracorporeal shockwave therapy, dry needling, stretches and specialised high load strengthening exercises. Lateral ankle sprains are very common among the active population and with proper professional guidance, can have serious long-term complications. Complications include fractures, recurrent sprains and ligamentous instability, resulting in surgery.
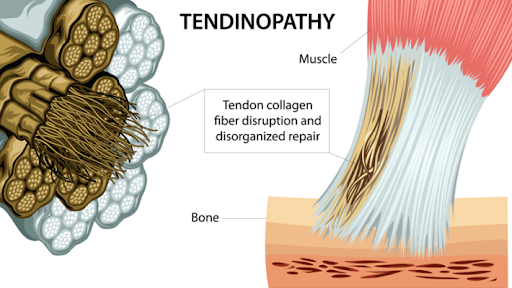
As a first point of call, it is important to get assessed by an experienced physiotherapist to get thoroughly assessed and diagnosed. Through history taking and physical examination, the physiotherapist will determine what ligaments have specifically been injured, the severity and whether an x-ray may be needed. Studies have shown that early mobilisation of a sprained ankle has significant benefits for improvements in pain, function and its long term stability. Physiotherapy treatment may include strategies to reduce swelling and inflammation, ankle taping/bracing, manual therapy to break up the scar tissue and an exercise rehabilitation program to help improve range of motion, strength, neuromuscular control and proprioception/balance. A high quality exercise rehabilitation program can get you back to what you were doing previously quickly and prevent injury recurrence. Tendinopathy is a generic term used to describe injuries to the tendon associated with inflammation and degeneration. It can be either characterised as a painful or pathological condition associated with overuse. Usually pain is associated with increased loads and a recognition that there has been a relative increase in inactivity. Pain is often reported as sharp early on and then becomes a dull ache weeks later. Pain may be present at the beginning of the activity then disappear during it, then returns on subsequent attempts of the activity.
Tendinopathies are common as they have a poor blood or nutrient supply compared to skeletal muscles. In fact, the oxygen consumption of tendons is about 7.5 times lower than skeletal muscles. A relatively low metabolic rate results in generally slow healing after injury. Common tendinopathies seen at Acland Street Physiotherapy include:
Tendinopathies generally respond well to physiotherapy treatment. This could include treatment techniques such as manual therapy, extracorporeal shockwave and eccentric strengthening exercises to improve the load capabilities of the tendon. |
Author
Archives
March 2024
|
Copyright Acland Street Physiotherapy © 2024


 RSS Feed
RSS Feed